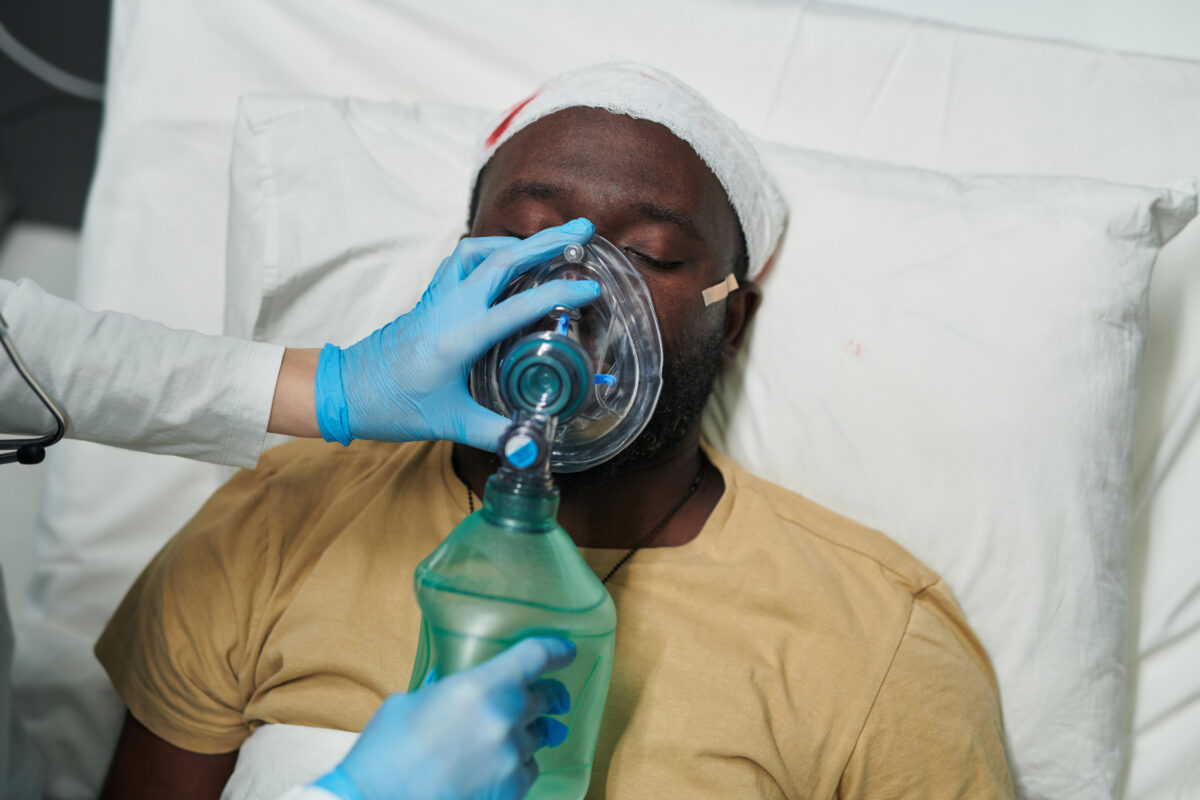
A break in brain activity is called a coma. When it occurs, you are unaware of what is happening around you and cannot wake up. In other words, it prevents consciousness. Coma can be mild to severe, depending on the cause it occurs. Fortunately, some coma causes are reversible and treatable. However, if a person experiences a coma, it is considered an emergency and requires immediate medical care.
What is Coma?
If a person experiences a coma, it means that the person is unconscious, unaware, and unresponsive to what occurs around them. In mild coma levels, it is considered that your brain does not work correctly. In most cases, a coma happens due to some health conditions that affect and damage your brain.
However, if you are with a person who is unresponsive or unconscious, you should immediately call 911. Otherwise, the coma can lead to serious complications or even death.
How Common are Comas?
Approximately 250 comas per 100,000 people happen in the U.S. and U.K. every year, according to research. In any case, uncertainty about the estimation accuracy persists because most of the comas are fast reversible by first responders. As a result, that person does not require a hospital.
Additionally, all patients with brain conditions can experience coma regardless of sex, age, race, ethnicity, or other factors.
Symptoms
Check below the most common coma symptoms:
- Lack of motor (movement) response – People with coma cannot consciously move and have some reflex responses. According to the reflexes you show, a doctor can determine how deep is your coma.
- Lack of eye response – When your eyes are closed and someone tries to open them, you do not have any reactions. However, certain eye reflex movements may happen including reacting to light, blinking, and turning when the head is moved but all these reflexes will not occur if you experience a coma that is very deep.
- Unconsciousness – A very deep sleep, which makes a person unable to wake up.
The Glasgow Coma Scale
This is the most common scale used to grade how severe a coma is. The Glasgow Coma Scale (GCS) has 3 categories and each one gets a score. The score of 15 is the highest possible and it means that you are aware and awake of your surroundings.
However, a score of 8, means you are in a coma. A score of 3 is the lowest possible and it means very deep coma. Check below 3 categories that GCS measures:
- Eye response (1-4)
- Motor response (1-6)
- Verbal response (1-5)
Causes
There are different health conditions that contribute to or provoke coma. Examples include:
- Hyperglycemia (very high blood sugar) and hypoglycemia (very low blood sugar) lead to diabetes-related coma
- Drugs and medical procedures such as anesthesia for surgery and medically induced coma
- Nonmedical and medical drug use
- Alcohol intoxication and poisoning
- Head injuries (such as traumatic brain injuries-TBI, concussions, and others)
- Brain bleeds
- Stroke including ischemic stroke in which blood flow decreases
- Poisons and toxins (including carbon monoxide, heavy metals, pesticides, and others)
- Infections (such as sepsis, encephalitis, meningitis, and others)
- Health conditions that provoke failure of the liver or kidneys
- Electrolyte imbalance (such as very low sodium-hyponatremia or very high calcium-hypercalcemia)
- Hypothermia (very low body temperature) and hyperthermia (very high body temperature)
- Intracranial hypertension (caused by hydrocephalus)
- Seizures (including status epilepticus)
Risk Factors
If any of the following cases occur, you are at higher risk of developing coma. Examples include:
- Metabolic diseases (such as type 1 diabetes, diabetes-related ketoacidosis-DKA also known as a complication of type 2 diabetes)
- Chronic health conditions including hypertension (high blood pressure), hyperlipidemia (high cholesterol levels in the blood), and others
- Substance or drug use (such as opioid and sedative medicines, alcohol use disorder, opioid use disorder, and any other substance use disorder)
- Head injuries (including concussions or TBIs due to not using protective gear or items)
- Heart diseases (such as irregular heart rhythms)
- Seizures or seizure-related diseases such as epilepsy or hypothyroidism (low thyroid gland function)
Complications
Those who are in a coma, need medical care 24/7 because they cannot move, bathe, and feed themselves. Furthermore, an individual should have a catheter placed to collect the urine and breathing assistance (mechanical ventilation to keep them breathing). However, certain complications can occur. For example:
- Pressure injuries (bedsores)
- Healthcare-associated infections (including ventilator-associated pneumonia-VAP, catheter-associated urinary tract infections-CAUTIs
- Tube feeding
- Muscle atrophy
- Blood clots (thrombosis)
- Delirium
- Tracheostomy (this procedure is required if the coma lasts more than 14 days)
Diagnosis
Physicians usually perform a neurological examination and use the GCS to verify how severe the coma is. It is important to diagnose quickly the underlying medical condition. Check below tests that will help to determine how severe the coma is:
- Electrocardiogram (ECG or EKG) – This test helps to verify heart rhythm.
- Electroencephalogram (EEG) – Your doctor will perform this test to determine your brain’s electrical activity. It also helps to identify the severity of your coma or detect coma-causing conditions including epilepsy and seizures.
- Diagnostic imaging – These tests include computed tomography (CT) scans and magnetic resonance imaging (MRI) scans. Imaging tests help to check your head for damage or injury.
- Laboratory testing of blood, urine, cerebrospinal fluid (CSF), and others – These are very helpful tests to determine the coma-causing factor. Laboratory tests help to determine blood sugar levels, electrolyte imbalances, organ failure, toxins and poisons, and others. They can also help to find infection symptoms.
Additionally, other tests are also possible depending on the coma itself. Healthcare providers are the best persons that will help to diagnose and treat this condition.
Treatment
The treatment usually varies among patients. It depends on the underlying cause, the severity of the condition, other existing diseases, prescription and nonprescription medicine use, and others. However, you should not administer or perform any medical procedures without a doctor’s recommendation because it may lead to unpleasant outcomes.
Furthermore, some treatments may start before knowing the exact cause of the coma. As a result, these treatments can help to stabilize the person and prevent the coma from worsening. Examples include:
- Insulin or Glucose – It helps to elevate or reduce the glucose levels in the blood and could reverse the coma quickly.
- Overdose-reversing Medicines – The caregiver or providers may give a person Naloxone. It is a medicine that helps to reverse an opioid overdose within 5 minutes.
Discuss with your healthcare professional about any treatment adverse reactions or complications.
Frequently Asked Questions
Can be coma prevented?
Yes, the following tips can help you to avoid or prevent the coma. Examples include:
- Treat your chronic health conditions
- Wearing safety equipment
- Eat a well-balanced diet
- Regular exercise and maintain a healthy weight for you
- Limit or avoid alcoholic consumption
- Do not use recreational drugs (such as cocaine)
For more details, talk with your doctor.
How long does a coma last?
In mild cases, it may last a few minutes but in severe cases, a person may experience a coma for years. Unfortunately, one coma complication is death, especially if a person does not get fast treatment.
What happens when you are in a coma?
This is a state of consciousness that is very similar to deep sleep. However, there is no sound or sensation that can wake up your brain. For example, a person cannot respond even to pain. A coma may occur due to different reasons including health conditions, head injuries or trauma, and others. Ask your physician in case you have any additional questions.