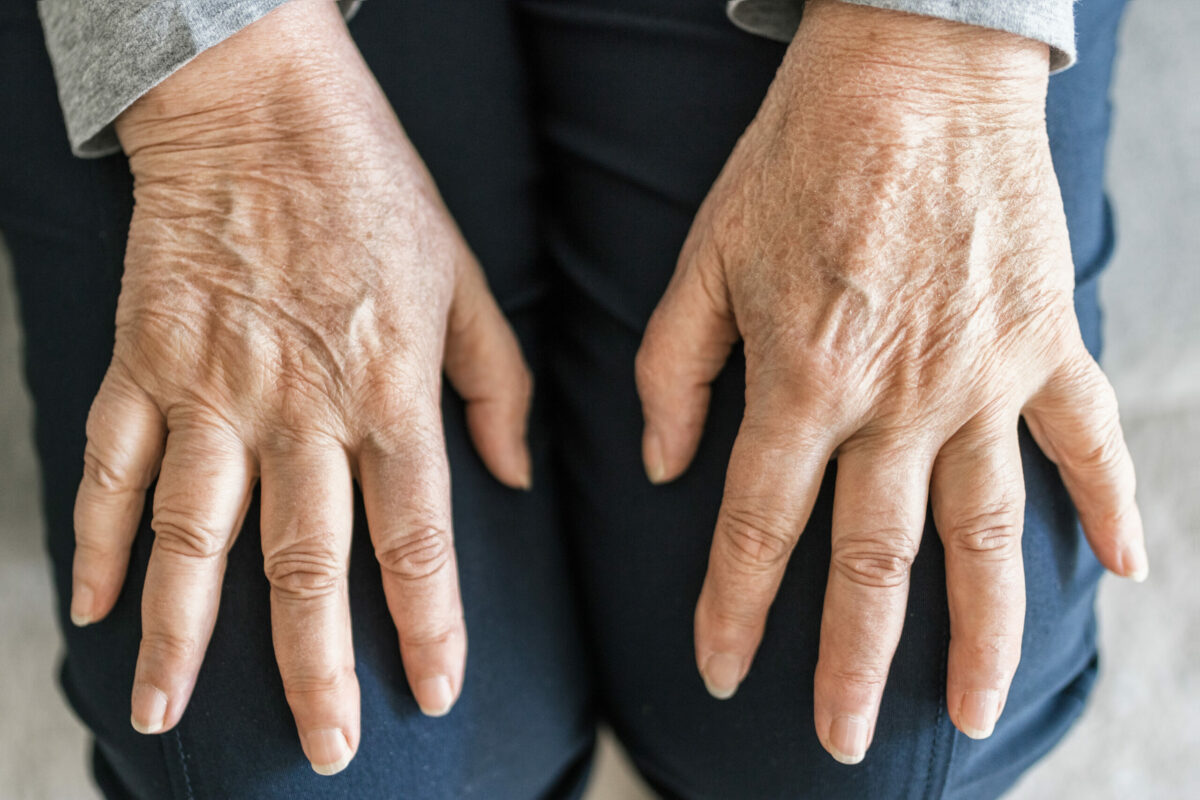
A health condition in which someone experiences joint pain and swelling caused by an infection in other body parts (commonly in the intestines, genitals, or urinary tract) is known as reactive arthritis. Mostly, it negatively affects ankles, feet, and knees. However, inflammation of the skin, eyes, and urethra (the tube that helps urine go outside the body). Another name for this health condition is Reiter’s syndrome.
In any case, reactive arthritis occurs quite rarely and symptoms go away within 1 year.
Symptoms
Commonly, symptoms of this condition appear within 4 weeks after an infection begins. Check below some examples:
- Pain and stiffness – Reactive arthritis usually impacts joints in the ankles, feet, and knees. However, you can also experience pain in the lower back, buttocks, or heels.
- Eye inflammation (conjunctivitis)
- Urinary issues (including discomfort while urinating and inflammation of the cervix or prostate gland)
- Tendons and ligaments inflammation
- Swollen fingers or toes (sometimes look like sausages)
- Skin problems such as mouth sores or rash
- Low back pain
Immediately visit a doctor if genital infections or diarrhea happen.
Causes
People commonly develop reactive arthritis when an infection occurs in the intestines, genitals, or urinary tract. Many people do not know they experience an infection because it provokes either mild or no symptoms at all.
There are different bacteria that provoke reactive arthritis. Moreover, some of them can be transmitted sexually and others are foodborne. Check below some examples:
- Chlamydia
- Shigella
- Yersinia
- Escherichia coli
- Clostridioides difficile
- Campylobacter
While the condition is not contagious the bacteria that provoked it can pass from person to person through contaminated food or sexual intercourse. Additionally, not everyone who gets the previous bacteria type develops reactive arthritis.
Risk Factors
Approximately all people can develop this arthritis type. Moreover, the following factors increase your risk. Examples include:
- Genetic factors – There are certain genes that have been linked to reactive arthritis. In any case, many people with this gene may never develop this condition.
- Sex – Both males and females are equally prone to getting this arthritis type. The only difference is that females are more likely to get this condition in response to foodborne infections while males are in response to sexually transmitted bacteria.
- Age – This is a condition that happens mostly in people aged between 20-40 years old.
Prevention
Genetics plays a role in reactive arthritis development. While you cannot change genetic makeup, it is advised to reduce the exposure to the bacteria.
Furthermore, you should store and cook foods at proper temperatures because it helps destroy many bacteria that provoke this arthritis type. For example salmonella, shigella, Yersinia, and campylobacter.
Practice safe sex to prevent sexually transmitted bacteria. In other words, it is advised to use condoms or dental dams during sexual activity.
Diagnosis
Physicians will perform a physical examination to check the joints for warmth, tenderness, and swelling and may ask you some questions about medical history and symptoms. They can also check you for eye inflammation and skin rashes. If they are not sure whether you have reactive arthritis or not, you may need to do some tests. Examples include:
Blood Tests
Commonly, blood tests are used to check for:
- Past or current infection
- Inflammation
- Antibodies linked to other arthritis types
- Genes that are associated with reactive arthritis
Joint Fluid Tests
Doctors will get a sample of joint fluid to test it for:
- White blood cell count that can help your doctor determine whether you have an infection or not.
- Bacterial infections (including septic arthritis)
- Uric acid crystals mean you have gout. This is a painful arthritis type that usually impacts the big toe.
Imaging Tests
Physicians can also perform X-ray tests of your lower back to determine if you have symptoms of reactive arthritis. This test can help your doctor to exclude other arthritis types.
Treatment
The treatment prescribed by doctors is different among patients because it depends on the underlying condition, the severity of the disease, and other factors. Commonly, the treatment goal is to reduce inflammation and treat the underlying infection. Check below some treatment options:
Medicines
Physicians usually prescribe antibiotics if you experience reactive arthritis due to bacterial infection. Check below some medications prescribed to lessen the symptoms:
- Nonsteroidal anti-inflammatory drugs (NSAIDs) – These medications are used to ease pain and inflammation in people with reactive arthritis. Commonly, doctors prescribe Indomethacin.
- Steroids – These medications come as injections, eye drops, or creams that are helpful in inflammation and pain management of the affected joints, eyes, or if you experience a rash.
- Rheumatoid arthritis medications – Some studies suggest that Sulfasalazine, Methotrexate, or Etanercept can help to reduce pain and stiffness in people with this arthritis type.
Physical Therapy
Sometimes, people need special exercise to support joints and muscles. For instance, strengthening exercises help to support affected joints by developing muscles around them. Talk with a physical therapist for more details.
Frequently Asked Questions
What products can trigger reactive arthritis symptoms?
If you are diagnosed with this arthritis type, it is advised to avoid the following products because they can trigger the symptoms. Examples include:
- Tobacco
- Alcoholic beverages
- Gluten
- Additives
- Advanced glycation end (AGE) products
- Fatty foods
- Carbohydrates
- Dairy products
- Sweets (an increased sugar consumption can worsen inflammation in the body)
What are the primary reactive arthritis causes?
Approximately all diagnosed reactive arthritis are provoked by sexually transmitted infections (STIs) such as chlamydia or bowel infection including food poisoning. However, not everyone who experiences previous infections develops this arthritis type.
What are the possible complications of reactive arthritis?
- Recurrent arthritis
- Chronic arthritis or sacroiliitis
- Ankylosing spondylitis
- Urethral stricture
- Aortic root necrosis
- Cataracts
- Cystoid macular edema
If you suspect any of them occur, immediately seek medical attention. In case you have any other questions, ask your healthcare professional.