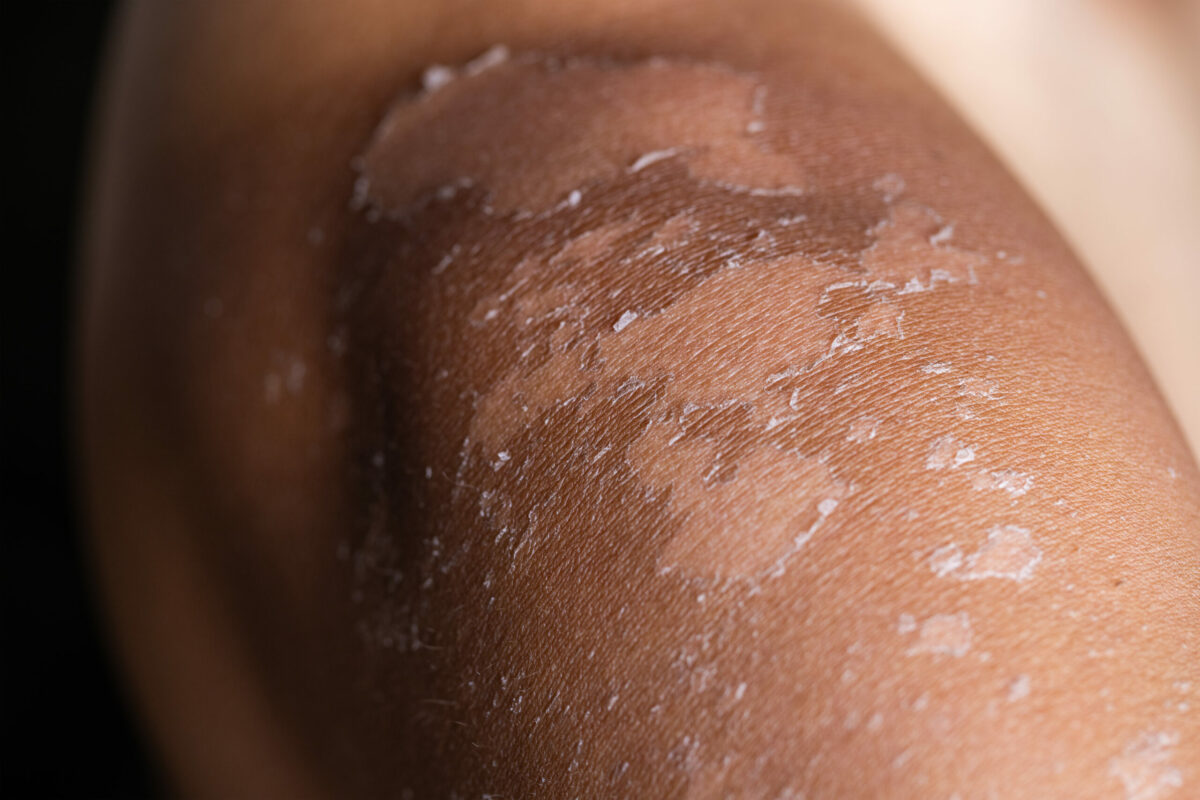
A group of skin conditions (about 30) that provoke dryness and scaling of the skin is called Ichthyosis. The name comes from the Greek word for fish because this condition makes skin look like scales on the fish. Others call this condition fish scale or fish skin disease.
Those who suffer from this skin disease lose the protective layer that maintains moist skin. It also produces new skin cells too fast or sheds old ones too slowly, which provokes a buildup of scaly and thick skin. Usually, most diagnosed ichthyosis forms are mild but it can be severe. In severe cases, this condition can negatively affect other organs.
Unfortunately, this condition has no cure but with early and proper treatment you can get rid of symptoms and improve the quality of life.
Ichthyosis Types
There are more than 30 types of this skin condition. Most of them are quite rare and mild while others can provoke problems inside the body. In most cases, ichthyosis appears with other medical conditions and syndromes. Check below for ichthyosis types:
- Ichthyosis vulgaris – This type impacts 1 in every 250 people and causes brown, white, or gray scales on the skin. It also is considered the most common ichthyosis type.
- X-linked recessive ichthyosis – Approximately 6,000 people suffer from this type and it mostly occurs in men and people assigned to male at birth (AMAB) than women and people assigned to female at birth (AFAB). This ichthyosis type usually begins between 3-6 months of age and tends to worsen over time. The common symptoms include scaling on the neck, face, trunk, and legs.
- Harlequin ichthyosis – Newborns usually suffer from this type and the symptoms include scaly and thick plates on the skin.
- Epidermolytic ichthyosis – It also occurs in babies and it leads to fragile and blistered skin throughout the body. Thereafter, the blisters disappear and the skin becomes scaly.
- Lamellar ichthyosis – A clear membrane (collodion membrane) occurs in newborns all over the body.
- Congenital ichthyosiform erythroderma – This skin condition is present at birth and collodion membrane also occurs.
- Erythrokeratodermia variabilis – It appears in babies after several months. It usually gets worse and spreads throughout the body as they grow. The skin often become rough, thick, or red on the arms, butt, legs, and face.
- Progressive symmetric erythrokeratoderma – This ichthyosis type commonly begins later in childhood and provokes red, scaly, and dry skin. It appears on the arms, legs, butt, face, ankles, and wrists.
Causes
This health condition can be inherited (genetic) or acquired due to other diseases or medicines you are using. If a person experiences a genetic ichthyosis, it means the condition passed from biological parents to biological children. In some cases, parents do not know they have this skin condition.
This disease usually appears in infancy or early childhood and if both parents have this mutated gene, you are more likely to develop a severe form of ichthyosis. However, some people may develop genetic ichthyosis without being inherited. It occurs due to a gene mutation during fetal development.
In any case, experts do not know the exact cause of acquired ichthyosis. It mostly happens in adulthood and along with other health conditions. For example:
- Kidney disease
- Hypothyroidism (underactive thyroid gland)
- Sarcoidosis (a disease that provokes inflammation inside the body)
- Cancers (such as Hodgkin’s lymphoma)
- HIV infection
Rarely, certain medications can trigger ichthyosis. Check below some examples:
- Cancer medicines (including Hydroxyurea and Vemurafenib)
- Protease inhibitors (medicines used in the HIV infection treatment)
- Nicotinic acid (helps to treat high cholesterol levels in the blood)
- Acid reflux medications (such as Cimetidine)
- Clofazimine (used in the leprosy treatment)
Symptoms
The symptoms appear differently among people because it depends on the type and severity of the ichthyosis a person experiences. In any case, about 95% of people experience ichthyosis vulgaris. The primary symptoms of this disease are dry and scaly skin that occurs in certain parts of the body including the trunk, stomach, buttocks, legs, face, and scalp.
In addition, the scales appear gray, white, or dark brown with thick or thin cracks between them. Dry and cold weather can worsen the symptoms. Check below for other ichthyosis vulgaris symptoms:
- Itchy skin
- Dirty-looking skin on the hands and feet
- Bumpy and rough skin on the thighs, butt, and arms usually looks like acne (keratosis pilaris)
- Trouble sweating
Some people may experience more severe symptoms including:
- Skin redness
- Blisters that can provoke wounds
- Peeling
- Itchiness
- Pain
- Hair loss
- Dry eyes
- Hearing problems
In most cases, people with ichthyosis often develop eczema. This condition usually appears in children before 5 years old and symptoms worsen over time until they reach puberty.
Diagnosis
In mild cases, this condition looks like simple dry skin. In case you experience discomfort due to dryness and scaling of the skin, it is recommended to visit a dermatologist. They usually ask you questions about symptoms and family history and perform a physical examination (looking at your skin, nails, and hair). If doctors are not sure whether you have ichthyosis or not, they can perform a biopsy and order you to do some tests including blood and saliva tests.
Treatment
Ichthyosis cannot be cured but proper treatment can lessen the symptoms and make you feel more comfortable. Physicians usually prescribe skin moisturizers, creams, ointments, and lotions. Moreover, it is advised to look for creams rich in lanolin, alpha hydroxyl acids, urea, or propylene glycol. In addition, the following tips can be used along with treatment to improve the symptoms. For example:
- Have more than one bath daily or hydrate your skin regularly
- Take baths that contain salt water because they can help to lessen burning, stinging, or itching of the skin
- Get rid of dead skin by rubbing it with a pumice stone or rough sponge
However, if you suffer from severe ichthyosis forms, physicians may prescribe oral medications (such as Acitretin and Isotretinoin). Previous medicines may provoke some adverse reactions including weakened bones, dry mouth, and stomach upset. In case you have skin infections, doctors recommend antibiotics.
Complications
The skin is a protective layer of the body and when it is scaling off, your risk of getting bacterial infection increases. Check below some ichthyosis complications:
- Skin infections
- Dehydration
- Sweat glands can be blocked, which often causes overheating
- Slower hair growth, especially on the scalp or hair loss
- Vision problems
- Hearing loss
- Brain and nervous system disorders
Moreover, children with this skin condition are more likely to develop other health problems. For example:
This skin condition can also provoke emotional problems because scaly skin impacts the way a person looks. As a result, those with ichthyosis may experience depression and low self-esteem.
Additionally, males with ichthyosis are at higher risk of testicular cancer, hidden testicles, and low sperm count.
Prevention
While this condition cannot go away, you can do different things that will help to feel better. For example:
- Regular skin moisturizing
- Stay cool because sweat and heat can make this condition worsen
- It is also recommended to use a humidifier
- You can also wear loose clothes produced from cotton or other fabrics that do not bother the skin
- Avoid detergents and other products that contain perfumes and dyes
Frequently Asked Questions
Does ichthyosis improve with age?
Many people noticed their ichthyosis gets better with age. However, they continue to treat the skin. This skin disease can cause other health problems in rare cases.
What is the most common ichthyosis type?
Ichthyosis vulgaris is the most common form of this skin condition.
What is the most common cause of acquired ichthyosis?
The medical conditions that could trigger ichthyosis include cancer (including lymphoma), sarcoidosis, infections (such as leprosy and HIV), long-term kidney failure, and others. Ask your healthcare professional if you have any questions.