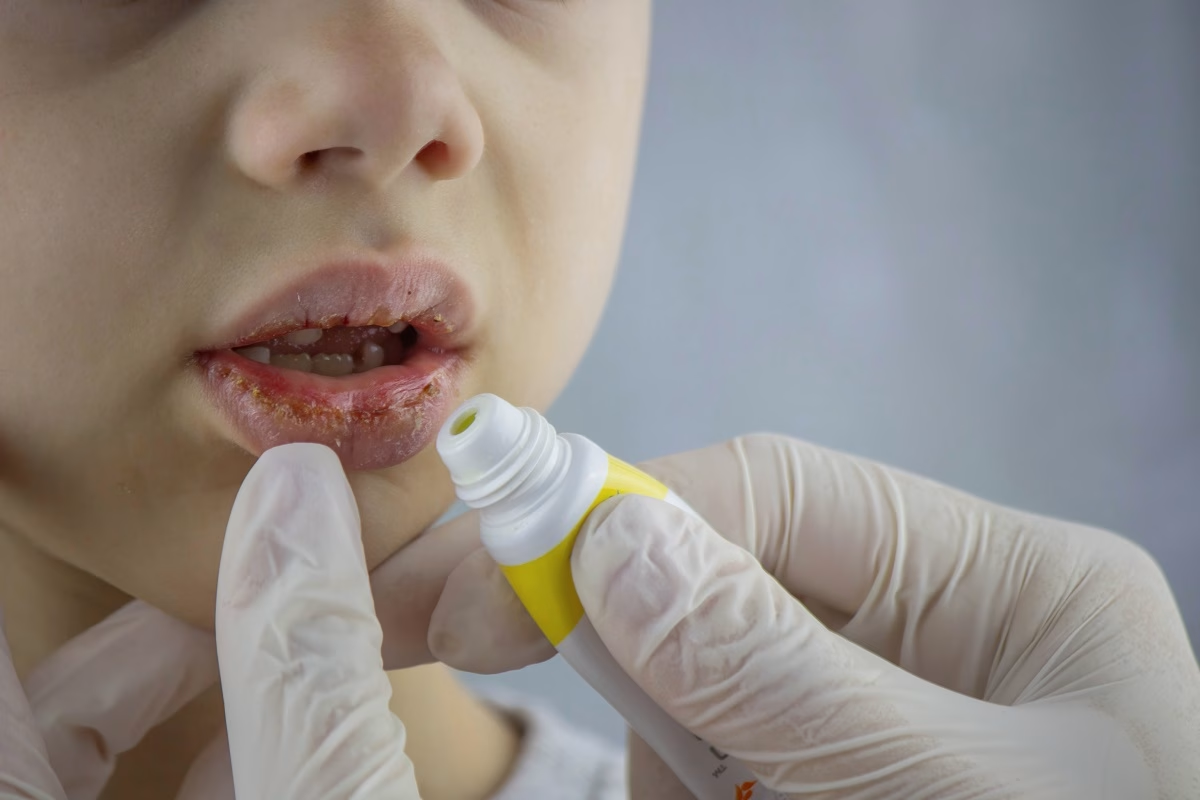
A chronic inflammatory disorder that affects the tissue lining inside the mouth is called oral lichen planus (OLP). The most common symptoms include skin changes that look similar to white patches or lacy threads on the inside of the cheeks and bright red gums. While this condition is not dangerous, most people need treatment to ease the symptoms.
Furthermore, this disorder often occurs for unknown reasons and may cause damage to the mucosa (thin tissue) lining your cheeks, gums, and tongue. This condition is not harmful and does not spread to other people (it is not contagious). If you notice symptoms similar to those caused by oral lichen planus, it is advised to see a dental care provider. While this condition cannot be cured, doctors may recommend some options to relieve the symptoms.
Types of OLP
Healthcare providers have divided this condition into 2 categories. These include:
- Reticular oral lichen planus – This is usually the mildest form of this disorder. It causes white spots, patches, or thread-like lesions inside the mouth. Moreover, these changes do not cause pain or discomfort.
- Erosive oral lichen planus – This is a more severe form of OLP, and it causes irritation to the gums and ulcers in one or more places inside the mouth. People with this type of OLP often experience pain when eating, drinking, or brushing their teeth.
Symptoms
The symptoms can be different among people with OLP. It depends on the type and severity of the condition, existing health problems, age, and other factors. Check below some symptoms often noticed in people with OLP:
- White spots or patches on the tongue or gums
- Ulcers on the gums, tongue, or the roof of the mouth
- Mild to severe pain, especially when brushing your teeth, eating, or drinking some foods (including acidic, crunchy, salty, or spicy foods).
- Bright red gums
- Web-like and white lesions inside the cheeks or on the tongue
Usually, people with OLP also have skin lichen planus. This type of condition may also cause an itchy rash on the genitals or scalp.
Causes
Healthcare professionals do not fully understand why this condition occurs. However, they think it is related to the immune system. Normally, the immune system produces antibodies that attack bacteria, parasites, and other germs that can make you sick. In people with OLP, the immune system attacks healthy cells inside the mouth. Furthermore, OLP occurs more commonly in people who administer the following medicines. For example:
- Antiparasitic medicines
- Antifungals
- Diuretics
- Beta-blockers
- Antiseizure medications
- Nonsteroidal anti-inflammatory drugs (NSAIDs)
In addition, sometimes people with the following conditions also develop OLP. Check below some of them:
- Hepatitis B
- Hepatitis C
- HPV (human papillomavirus)
- Primary biliary cirrhosis
However, more research is needed to understand the link between previous disorders and OLP.
Triggers
In most cases, doctors recommend finding and avoiding triggers that cause symptom flare-ups. Check below the most common triggers for people with OLP:
- Certain medicines (such as beta-blockers)
- Mouth injuries or infections
- Stressful situations
- Mental health problems (such as depression, anxiety, and others)
- Dental problems (including a misaligned bite or jagged teeth)
- Allergic reactions to foods, toothpaste, or floss, or other dental materials
Risk Factors
While it is not possible to determine the exact cause of OLP, doctors have identified some factors that could increase your risk of developing it. Check below some examples:
- Autoimmune disorders – Usually, this condition is linked to other immune-related disorders.
- Hepatitis C – This is a possible trigger of the OLP.
- Systemic disorders – These include thyroid disorders, liver disease, diabetes, hyperlipidemia, and others.
- Prolonged stress
- Allergies
- Sex – Females are more likely to develop OLP compared to males.
- Age – This condition often occurs in people between the ages of 30 and 70.
- Poor oral habits, mechanical trauma of the teeth, and allergy to dental materials
What Are The Potential Complications of Oral Lichen Planus?
People with oral lichen planus may also experience some complications, especially if they do not get treatment or develop the more severe form of the disease. Check below some examples:
- An increased risk of yeast and bacterial infections
- Damage to the mucosa
- Weight loss (this complication often occurs when eating hurts too much)
- Oral cancer – According to some research, about 1% to 4% of people with OLP develop oral cancer. However, more research is needed to understand why some people develop this type of cancer while others do not.
- Scarring
- Increased sensitivity to certain foods (especially acidic or spicy foods)
This document does not contain all possible complications of OLP. In any case, you can talk with your physicians about ways to reduce the risk of developing them. Additionally, OLP cannot be prevented because doctors do not fully understand why it happens.
Diagnosis
While sometimes doctors may diagnose OLP during a mouth examination, in most cases, they will perform a biopsy to confirm or rule out this condition. During this test, doctors will take a small amount of affected tissue for testing.
Treatment
This condition cannot be cured. That’s why doctors prescribe treatments to relieve the symptoms and improve your quality of life. Check below some options often recommended by doctors for people with OLP:
Medicines
The following medications are often prescribed by doctors when you have symptoms. Some of them are used to reduce the immune system reaction. For example:
- Corticosteroids – Physicians often recommend a gel or ointment to rub on the lesions. When these medicines do not work, you may get a prescription for a shot or a pill that is administered by mouth.
- Calcineurin inhibitors – This group of medicines is used when corticosteroids do not help. In most cases, physicians recommend an ointment to rub on the lesions.
- Painkillers – These are specific medicines that help relieve the pain caused by this condition. Usually, physicians recommend over-the-counter (OTC) pain relievers (such as Acetaminophen), but if they do not help, you may get a prescription for Lidocaine to numb the pain.
Lifestyle Changes
The following lifestyle changes may also help ease the symptoms. For example:
- Avoid spicy, salty, crunchy, and acidic foods
- Avoid alcoholic drinks and tobacco products
- Use a soft-bristled toothbrush or an electric toothbrush
- Manage stress
- Avoid medicines that cause flare-ups
- Use mild and unflavored toothpaste and dental floss without mint, cinnamon, or sodium lauryl sulfate
Recovery
In most cases, people notice improvements in their symptoms within a month after starting the treatment. When topical medicines are not an option, you can notice improvements within 2-3 shots. Additionally, oral medicines often provide improvements within several weeks.
Frequently Asked Questions
When should I see my healthcare provider?
If you notice unusual patches or lesions inside the mouth, it is advised to see a doctor for testing. In rare cases, these changes can indicate oral cancer. Furthermore, people diagnosed with OLP should have regular dental check-ups to prevent serious complications.
What can be mistaken for oral lichen planus?
There are some conditions that are often mistaken for oral lichen planus. These include:
- Yeast infections (such as oral thrush)
- Leukoplakia
- Erythroplakia
- Lichenoid dysplasia
- Proliferative verrucous leukoplakia
- Lupus erythematosus
- Mucous membrane pemphigoid
This document does not contain a full list of disorders that can be mistaken for oral lichen planus.
What is the cause of oral lichen planus?
The exact cause of OLP is not known, but experts think it is an autoimmune disorder. In general, autoimmune conditions occur when the immune system attacks its own healthy cells instead of viruses, bacteria, and other germs. Ask your healthcare provider if you have additional questions.