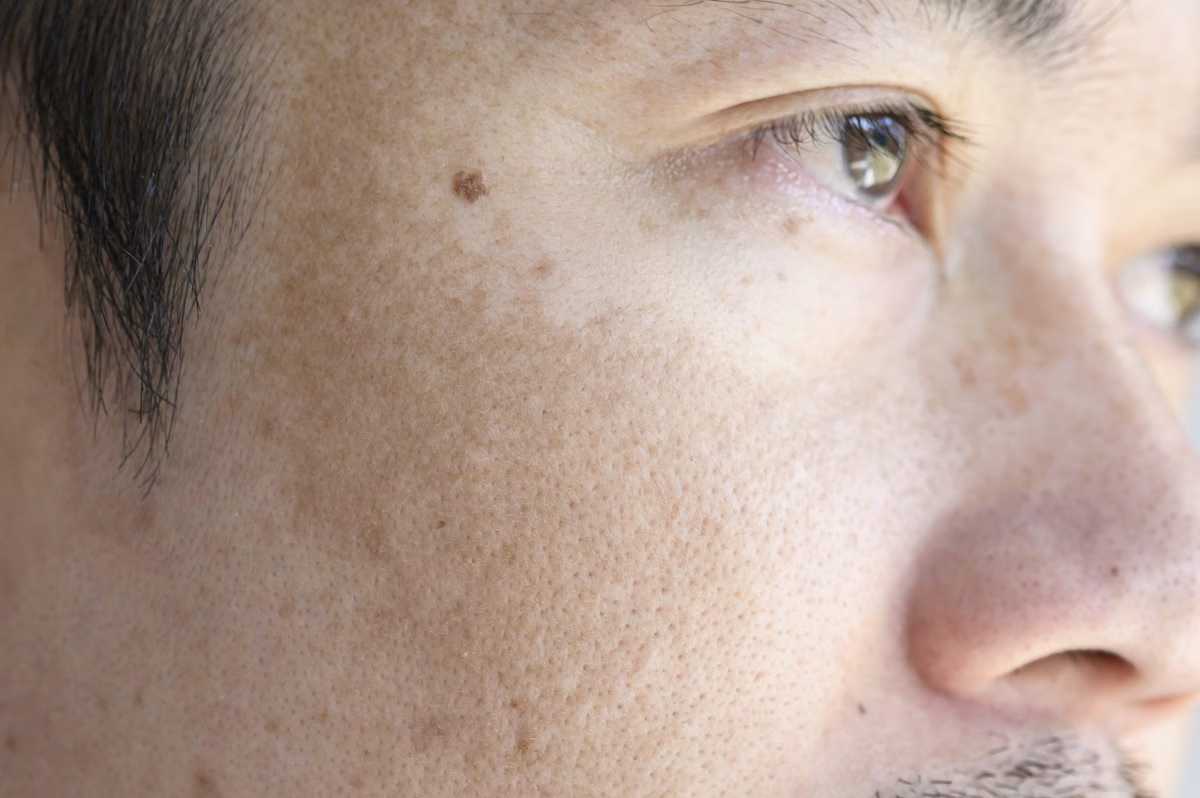
A skin condition that causes brown or blue-gray patches or freckle-like spots is called melasma (less commonly called cholasma). Sometimes, it is called the “mask of pregnancy”, and it occurs due to overproduction of the cells that make the color of the skin. Most of the time, this condition is harmless, and it disappears after several months.
In general, melasma is a common skin condition that often causes symptoms on the face (including the cheeks, upper lip, and forehead) and forearms. The symptoms of this condition often darken and lighten over time, and may get worse in the summer and improve in the winter. While it mostly occurs on the face, it may also affect other parts of the body. For example, body parts that are exposed to sunlight (including the back, neck, and arms).
Generally, this is a very common skin disorder, especially in pregnant women. It affects about 15% to 50% of pregnant women and 1.5% to 33% of the population. Mostly, it affects women during their reproductive years and often begins between the ages of 20 and 40.
Types of Melasma
Physicians have divided this condition into 3 categories based on the depth of the pigment. These include:
- Epidermal – This type was a dark brown color with a well-defined border. Usually, it appears obvious under black light and sometimes responds well to treatment.
- Dermal – In such cases, it causes light brown or bluish color spots with a blurry border. Commonly, it appears differently under black light, and it is difficult to treat.
- Mixed melasma – This is the most common type of melasma, and it causes both bluish and brown patches that show a mixed pattern under black light. Treating mixed melasma can also be challenging.
Physicians usually use a Wood’s lamp that emits black light to determine the depth of the pigment.
Is Melasma Cancerous?
No, this skin condition is not malignant (cancerous), a sign of cancer, or a skin disease that may turn into cancer. Unfortunately, there are some tips of skin cancer that mimic the symptoms of melasma. That’s why it is recommended to see a doctor if the symptoms appear. While melasma is a harmless condition that does not cause pain, itching, or discomfort, it is a chronic (long-term) disorder. Some people may have symptoms of melasma for years of their entire lives.
Symptoms
People who develop melasma often experience light brown, dark brown, and/or bluish patches or freckle-like spots on the skin. In some cases, these patches can become inflamed or red. The symptoms of this condition may appear in the following 6 parts of the body or in multiple parts at the same time. For example:
- Brachial – (On the shoulders and upper arms)
- Centrofacial – (On the forehead, cheeks, nose, and upper lip)
- Lateral cheek pattern (in such cases, the spots appear on both cheeks)
- Malar (on the cheeks and nose)
- Mandibular (on the jaw line)
- Neck – The symptoms of melasma often appear in people over 50 years old on all sides of the neck.
If you experience spots or freckle-like patches on the skin, do not hesitate to visit a doctor for a diagnosis, because there are some skin cancers that cause similar symptoms.
Causes
In general, there are two primary causes of melasma. These include radiation (whether ultraviolet, visible light, or infrared) and hormones. In most cases, people develop melasma due to infrared radiation from the sun. Check below for other possible causes of this skin disorder:
- Antiseizure medicines – These medications are used to prevent seizures, but may also cause melasma. Commonly, people who administer Clobazam develop this skin condition.
- Contraceptive therapy (also known as birth control) – Melasma is also more common in people who use oral contraceptive pills that contain Estrogen and Progesterone.
- Estrogen/Diethylstilbestrol – This is a man-made (synthetic) form of Estrogen that is often prescribed by doctors to treat prostate cancer.
- Genetics – Approximately 33% to 50% of people have a family history of the disease.
- Hypothyroidism – This is a condition in which the thyroid gland is underactive and produces reduced amounts of thyroid hormones. Additionally, people who have melasma are more prone to thyroid disorders.
- LED screens – This skin condition can even be caused by LED lights from your TV, laptop, cell phone, and tablet.
- Pregnancy – Doctors do not know why pregnant women develop this condition, but some experts think that increased Estrogen levels contribute to it.
- Hormones – Healthcare professionals noticed that Estrogen and Progesterone play a role in melasma. For instance, some postmenopausal women develop melasma due to the Progesterone they administer.
- Makeup (cosmetics) – There are some cosmetics that may trigger a phototoxic reaction.
- Phototoxic drugs (medicines that make you more sensitive to sunlight) – Examples include nonsteroidal anti-inflammatory drugs (NSAIDs), antibiotics, diuretics, retinoids, hypoglycemic medicines, antipsychotic drugs, targeted therapies, and others.
- Skin care products – A lot of people use skin care products that can cause irritation to the skin and cause melasma.
- Soaps – Avoid scented soaps because they can cause or worsen an existing skin disorder.
- Tanning beds – You should know that ultraviolet (UV) light produced by tanning beds may also cause damage to your skin.
Do Certain Foods Affect Melasma?
Nowadays, there is no evidence that foods directly cause, cure, or worsen melasma. In any case, you can consider the following foods to keep your skin healthy. These include:
- Almond milk
- Mushrooms
- Oily fish
- Meat
- Milk
- Eggs
- Orange juice
- Yogurt
How to Prevent Melasma?
While some people can prevent this skin condition, you cannot avoid genetics. If you develop melasma due to genetic changes (mutations), it is not possible to reduce the risk or prevent it. However, you can take steps to prevent worsening of the condition. Discuss it with your doctor for more details.
Diagnosis
Like many other conditions, the diagnosis of melasma begins with a physical examination in which doctors will check for irregularities linked to the disease. After that, they will use a Wood’s lamp to see changes in the skin’s color. In most cases, doctors will also examine the thyroid gland because thyroid disease is frequently associated with melasma. However, to confirm or rule out melasma, physicians often perform a skin biopsy. During this test, they will take a sample of the affected skin for testing. Usually, skin biopsies help reveal the following things. For example:
- Dendritic pigmented melanocytes
- Melanin in the basal keratinocytes, suprabasal keratinocytes, and melanin in the dermis within melanophages.
- Solar elastosis and elastic fiber fragmentation
Once you are diagnosed with melasma, doctors may use the Melasma Area and Severity Index (MASI) to determine the severity of the skin condition.
What Health Conditions Can be Mistaken for Melasma?
In some cases, this condition can be mistaken for other skin disorders because it causes similar symptoms. These include:
- Acnitic lichen planus and lichen planus
- Drug-induced pigmentation
- Guttate hypomelanosis
- Hydroquinone-induced exogenous ochronosis
- Nevus or Hori
- Lentigo (also known as age spots)
- Post-inflammatory pigmentation
Treatment
First, you should make sure you avoid things that could make the symptoms worse. For example, avoiding the sun, tanning beds, LED screens, irritating soaps, and birth control pills. In any case, you can use a SPF of 30-50 that should be applied every 1.5 hours if you are exposed to the sun.
Healthcare professionals often prescribe topical therapy using tyrosinase inhibitors to treat melasma. Check some examples below:
- Azelaic acid – This medicine should be applied twice a day, and it comes in gels, creams, and lotions. Moreover, it is safe for pregnant women to use.
- Cysteamine – According to a study of 50 people who use this medicine, have shown that it is more effective than a placebo.
- Hydrocortisone (a topical corticosteroid) – Doctors often prescribe it to fade skin color caused by melasma.
- Hydroquinone – This medicine comes in creams and lotions, and it should be applied directly onto the melasma patches.
- Methimazole – This is an antithyroid cream or an oral tablet that helps improve symptoms.
- Soybean extract – This product often helps reduce the transfer of color from the melanocytes to the skin cells.
- Topical alpha hydroxy acid – This is a special cream used to peel off epidermal pigments.
- Tranexamic acid – This medicine comes in creams, injections, and oral medicines, and it helps relieve the symptoms caused by melasma.
- Tretinoin – This is a prescription topical retinoid used to treat symptoms of melasma and dermatitis, but cannot be used during pregnancy.
Check below for other agents that are being studied to improve melasma:
- Arbutin
- Ascorbic acid (vitamin C)
- Glutathione
- Licorice extract
- Kojic acid
- Mequinol
- Runicol
- Zinc sulfate and others
Frequently Asked Questions
Can melasma be raised on the skin?
In most cases, melasma is flat, but if you develop raised bumps on the skin, it may indicate another skin disorder.
Is there a cure for melasma?
The chances of curing this condition are different among people. It often depends on the genetic factor, the severity of the condition, age, gender, existing health problems, and others. For example, some people may develop chronic (long-term) melasma while others get rid of this condition even without treatment. For more details, discuss it with your doctor.
Are there any procedures that can help with melasma?
Yes, physicians may recommend some procedures along with the previous medicines to manage the symptoms of melasma. For example:
- Chemical peel – During this procedure, dermatologists will put a chemical on the skin that makes it peel. Thus, it helps regenerate the skin.
- Light-based procedures – Sometimes, doctors may also recommend intense pulsed light, non-ablative fractionated lasers, and low fluence Q-switched lasers to improve the symptoms.
If you have any other questions, ask your healthcare provider.