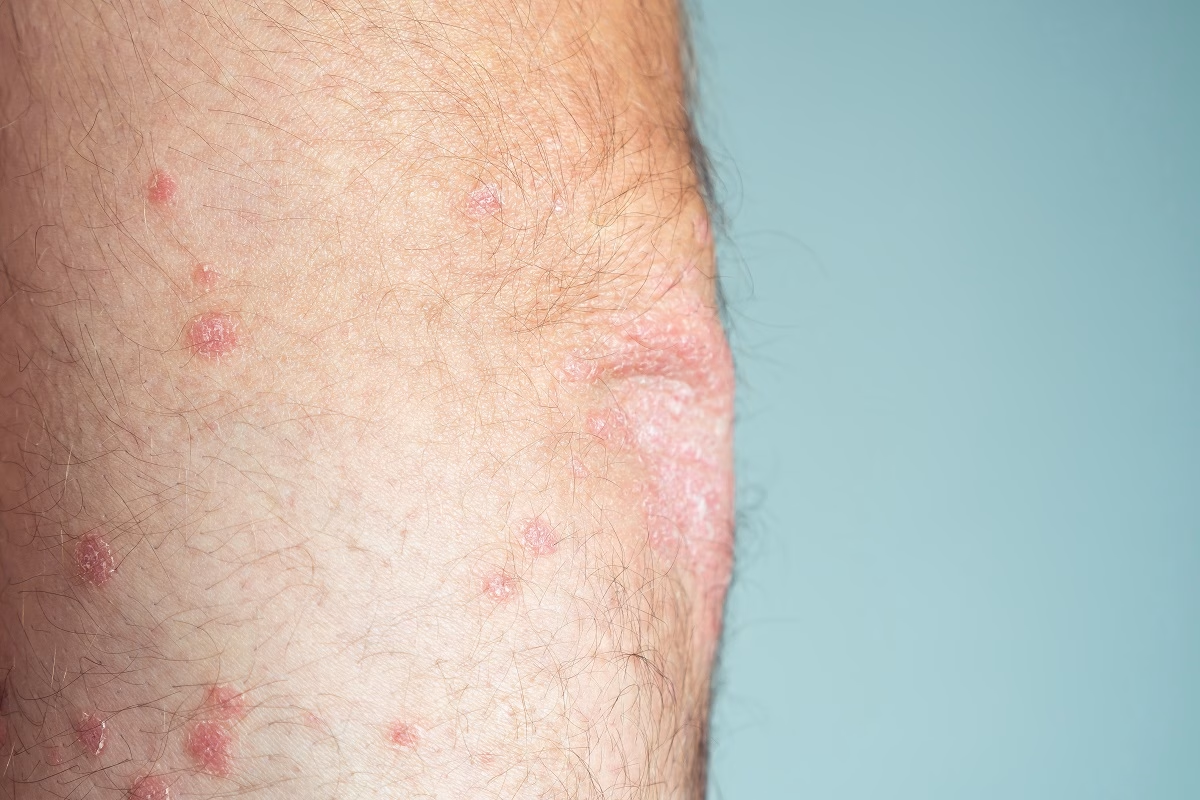
A chronic (long-term) skin disorder that causes small and discolored bumps or blisters on the skin is called pyoderma gangrenosum. These blisters often join together and form large open sores (ulcers). Healthcare providers do not fully understand why it occurs, but it is often linked to some autoimmune disorders or an earlier skin injury. Commonly, it is quite difficult to diagnose it because the symptoms resemble other health conditions. However, there are some medicines and procedures that may help ease the symptoms. In most cases, people experience scarring.
While a mild form of pyoderma gangrenosum may cause only one ulcer, in more severe cases, people may develop multiple or many open sores that are painful. Mostly, there is a link between this skin disorder and other systemic diseases.
This condition occurs rarely and affects about 1 in every 100,000 people in the U.S.
Is Pyoderma Gangrenosum Life-threatening?
According to some studies, about 70% of people who develop this condition also have other health conditions at the same time (comorbidities). For example, a combination of pyoderma gangrenosum and other systemic disorders, including rheumatoid arthritis, inflammatory bowel disease (IBD), and blood disorders. In general, the mortality rate is about 30%, especially without treatment.
Symptoms
In most cases, this chronic skin disease negatively affects the lower extremities (legs), but it may also occur on the arms, genitals, and neck. Check below some general symptoms of pyoderma gangrenosum:
- Pus-filled, discolored, and small blisters that may become large quite fast
- Open sores (ulcers) with distinct and raised borders
- Inflammation and pain around the sores
- Fever
- Joint pain
In severe cases, people may experience large, deep, and very painful open sores. It is recommended to contact your healthcare professional if any of the previous symptoms occur.
Causes and Risk Factors
Healthcare providers do not fully understand why this condition occurs, but about 50% of people with pyoderma gangrenosum have other disorders, such as leukemia, lymphoma, ulcerative colitis, rheumatoid arthritis, or Crohn’s disease. Furthermore, this disorder may also appear after an injury to the skin (such as trauma or surgery). When this condition appears near a surgical opening (also known as the stoma site), it is called peristomal pyoderma gangrenosum.
In addition, physicians have identified some factors that could increase your risk of developing this condition. These include:
- Age – While this condition may affect people at any age, it is mostly diagnosed between the ages of 20 and 50.
- Sex – Pyoderma gangrenosum usually negatively affects females.
- Rheumatoid arthritis
- Some types of cancer – These include leukemia, lymphoma, and others
- Crohn’s disease
- Ulcerative colitis
- Joint diseases
- Sarcoidosis
- Sjogren’s syndrome
- Myeloproliferative disorders
- Endocrine and metabolic diseases (such as diabetes)
- Obesity (excessive body weight)
- Genetics – For example, PAPA and PASH syndromes
- Misuse of recreational drugs
In addition, this condition is not contagious. It means pyoderma gangrenosum cannot spread to other people through skin-to-skin contact.
What Are The Possible Complications of Pyoderma Gangrenosum?
People with this condition may also experience some complications, especially if they do not get treatment. Check below some examples:
- Infections
- Severe pain
- Scarring
- Post-inflammatory skin color changes (such as hyperpigmentation or hypopigmentation)
- Loss of mobility
- Increased mortality risk
- Mental health problems (such as depression and anxiety)
- Isolation
- Reduced quality of life
This article does not contain a complete list of pyoderma gangrenosum complications. However, you can consult with your healthcare professional about measures to reduce the risk or even prevent the previous complications.
How to Prevent Pyoderma Gangrenosum?
This condition cannot be prevented because physicians do not fully understand why it happens. However, it is recommended to see a doctor immediately if you notice any symptoms that resemble pyoderma gangrenosum. This condition usually advances quickly and leaves permanent scars. You should also inform your doctor if you have other health problems (such as blood cancer, autoimmune disorders, and others).
Diagnosis
Usually, it is challenging to diagnose this condition because it causes symptoms similar to other health conditions, and there is no specific test that can confirm it. That’s why doctors perform some tests to rule out other disorders that cause the same symptoms. Check some conditions below:
- Systemic lupus erythematosus
- Skin cancers
- Sweet syndrome
- Inflammation of the blood vessels located near the skin
Commonly, doctors perform the following tests to rule out or confirm this condition. For example:
- Blood test
- Bone marrow sampling
- Rectal examination (proctoscopy)
- Biopsy
- Colon examination (colonoscopy)
Treatment
Mostly, doctors prescribe different treatments for people with these skin disorders because it depends on several factors. These include the severity of the condition, age, overall health, and preferences. While a mild form of pyoderma gangrenosum is treated with topical medicines (creams or ointments), in more severe cases, doctors may prescribe oral medicines. According to some studies, newer medications (biologic agents) may help. To prevent permanent scarring, early diagnosis and proper treatment are very important.
Medicines
- Corticosteroids – This group of medicines is primarily used to reduce inflammation. It may help relieve the symptoms. However, it may cause some adverse reactions, including appetite changes, weight gain, mood swings, acne, and sleep disturbances (insomnia).
- NSAIDs (nonsteroidal anti-inflammatory drugs) – These medications are used to relieve aches and pains. Doctors often recommend Ibuprofen or Aspirin. In some cases, people may have some side effects, such as bloating, abdominal (belly) pain, nausea, vomiting, diarrhea, or constipation.
- Silver Sulfadiazine skin cream – This is an antibiotic cream often prescribed by doctors to treat second- or third-degree burns. It also helps prevent or treat serious infections. The most common adverse reactions of this medicine are fever, itching, skin rashes, increased sensitivity to light, and chills.
If you develop a severe form of pyoderma gangrenosum, doctors may recommend the following treatments. These include:
- Immunosuppressants – This group of medicines is usually used to reduce the activity of the immune system, which helps relieve the symptoms. Doctors often prescribe Cyclosporine or Mycophenolate.
- Biologic agents – These medicines are used to target specific inflammatory proteins. Physicians often recommend Infliximab, Adalimumab, and Ustekinumab.
- Hyperbaric oxygen therapy – This therapy is often recommended by doctors to treat wounds and other diseases by supplying you with 100% oxygen inside a specific chamber. It also allows you to get more oxygen as you breathe.
- Skin graft – This is a type of surgery used to transplant healthy tissue from one part of the body to the affected part of the body.
Frequently Asked Questions
How long does it take pyoderma gangrenosum to heal?
In general, it is difficult to treat this condition. Even with proper treatment, the wound may heal within weeks or even months.
How does pyoderma gangrenosum affect my body?
This condition often causes small and discolored bumps and inflammation on the skin. Without early diagnosis and proper treatment, it may lead to permanent scarring. These ulcers usually appear on the legs, ankles, and feet, but may also affect the neck, arms, and other parts of the body. Usually, small bumps quickly join together and form large and painful open sores.
Is pyoderma gangrenosum an autoimmune disease?
Doctors are not sure that this condition is an autoimmune disorder, but it is often linked with certain autoimmune diseases. An autoimmune condition occurs when the immune system attacks healthy cells instead of bacteria, viruses, and other germs that can make you ill. In some cases, this condition improves once you get treatment for an existing systemic disease. Ask your healthcare provider if you have additional questions.