A congenital heart defect that is present in newborns at birth, in which the functional pulmonary valve is missing, is called pulmonary atresia. Normally, the pulmonary valve helps blood get into the pulmonary artery, which then goes to the lungs, where it gets fresh oxygen. When this valve develops improperly or is missing, the blood is not able to get enough oxygen for the body’s needs.
In general, this condition occurs in about 1 in 6,700 live births in the U.S. Moreover, babies with this condition may also have other heart problems. These include:
- Underdeveloped right ventricle and tricuspid valve (the valve that connects the right atrium and right ventricle).
- An abnormal opening (the foramen ovale) between the right atrium and left atrium. In normal circumstances, this opening should close shortly after birth. When it closes, oxygen-poor blood can pass from the right atrium to the left atrium, where it goes through the left ventricle to the aorta.
- Problems with a dividing wall (also known as a septum) between the right and left sides of the heart. Normally, this wall correctly directs the blood.
In healthy people, the right part of the heart sends blood to the lungs to get fresh oxygen, and then the left side of the heart moves this oxygen-rich blood to all body tissues and organs through the aorta (the primary artery in the heart). However, in people with pulmonary atresia, the dividing wall problem is often called pulmonary atresia with a ventricular septal defect (VSD). This condition causes the oxygen-rich blood to mix with oxygen-poor blood.
Symptoms
Usually, the symptoms of this congenital heart defect appear in the first few hours or days after birth. You may notice your child experiences cyanosis (blue fingers, toes, and lips) due to a lack of oxygen in the blood. This is one reason why healthcare professionals consider pulmonary valve atresia a cyanotic heart problem. However, this condition may also cause other symptoms. These include:
- Fatigue (extreme tiredness)
- Poor feeding
- Irritability
- Dyspnea (shortness of breath)
- Fast breathing
- Clammy, cool, or pale skin
Immediately contact your healthcare professional if you notice your child has any of the previous symptoms.
Causes and Risk Factors
Experts do not fully understand why this condition occurs, but it often appears during the first 8 weeks of a fetus’s development in the uterus. Physicians think genetic factors (such as abnormal genes or chromosomal defects) could play a role in congenital heart defects. In some cases, babies with DiGeorge’s syndrome also develop pulmonary atresia.
Physicians have also identified some factors that may increase your child’s risk of developing this congenital heart defect. These include:
- Family history of congenital heart defects
- Advanced maternal age
- Unmanaged diabetes in the mother
- Teratogenic drugs during pregnancy
- Use of tobacco and alcoholic products during pregnancy
- Environmental exposure to toxins
- Infections during pregnancy, including German measles (also known as rubella)
Complications
Children with pulmonary atresia may also experience some complications, especially if the condition is left unmanaged. Check below some of them:
- Arrhythmia (irregular heart rhythm)
- Pulmonary artery stenosis (this is a condition in which the pulmonary artery becomes narrowed)
- Collateral circulation (abnormal connections between blood vessels in the chest)
- Liver disease
- Delayed growth and development
- Heart failure
- Infectious endocarditis
- Stroke
- Seizures
The previous list does not contain a full list of pulmonary atresia complications. However, you can consult your healthcare professional about ways to reduce the risk or even prevent them.
Diagnosis
Normally, healthcare professionals should perform standard screenings to check on the health of the fetus. If they suspect something, they may perform an ultrasound. This is a harmless imaging test used to examine the fetal heart. After birth, they may also listen to your baby’s heart and lungs to determine if any problems are present. Check below some tests often used to confirm or rule out pulmonary atresia:
- Pulse oximetry – During this procedure, doctors will attach a specific device to the baby’s big toe to determine how much oxygen is in their blood.
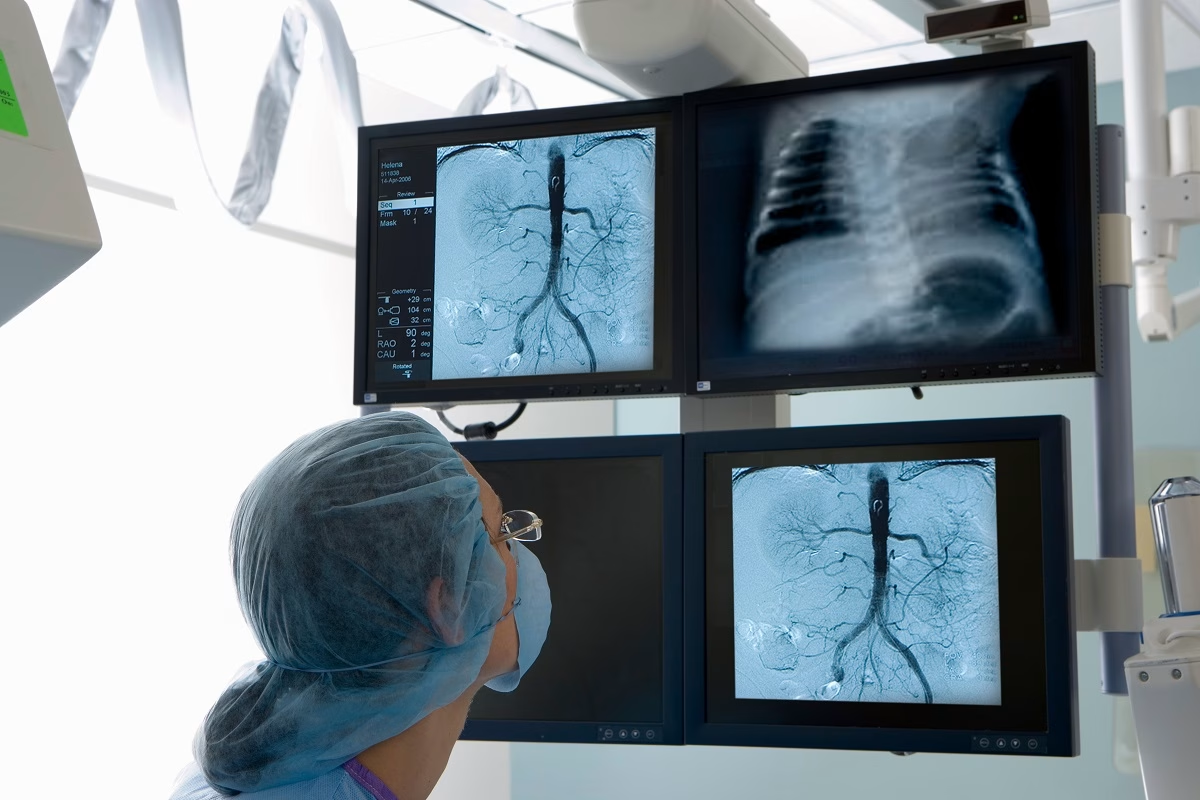
- Chest X-ray – This test helps get pictures of the inside of the baby’s chest.
- Electrocardiogram (ECG or EKG) – This is a harmless test used to measure the electrical activity of the heart. It usually helps identify arrhythmia (irregular heart rhythm) or heart muscle stress.
- Echocardiogram – This is another imaging test that uses sound waves to make a moving picture of the baby’s heart and its valves.
- CT (computerized tomography) angiogram – This test uses a contrast dye to show the baby’s heart on X-ray images from scans.
Treatment
The treatment is often different among people with pulmonary atresia because it depends on how the condition affects your child, their general health, age, and medical history. While some temporary options include medicines and procedures, most people with pulmonary atresia require surgery to improve blood flow to the lungs. Unfortunately, there is no way to cure this congenital heart defect, but with treatment, the condition may improve.
Medicines
Usually, doctors recommend an intravenous (IV) medicine with Alprostadil to prevent the ductus arteriosus from closing. It helps oxygen-poor blood flow from the baby’s aorta to the pulmonary arteries, where it gets fresh oxygen.
Procedures
These procedures involve a stent that is placed inside the ductus arteriosus to make sure it remains open. In some cases, doctors may recommend a septostomy. During this procedure, they will enlarge the opening in the wall between the baby’s upper chambers of the heart. Therefore, it improves blood flow to their lungs.
Surgery
There are some types of surgery that doctors may recommend for people with this condition. However, it depends on the size of the right ventricle and pulmonary artery, and the ability of the right ventricle to pump blood. When your child has pulmonary atresia and VSD, doctors may close the baby’s ventricular septal defect by placing a donated artery and valve between the child’s right ventricular and pulmonary artery. As a result, it helps improve blood flow through the right ventricle into the pulmonary artery and then to the lungs.
In people with this congenital heart defect without VSD, the right ventricle often develops improperly. That’s why they often need a series of 3 surgical interventions in their first years of life. The following options are open-heart surgeries that help redirect the flow of oxygen-poor blood directly to the pulmonary artery. Check some options below:
- BTT shunt – This procedure involves placing a shunt or tube that is placed from the baby’s subclavian artery to their pulmonary artery.
- Glenn procedure – This treatment is used to remove the shunt between 4 and 8 months of age and connect the superior vena cava to the right pulmonary artery.
- Fontan procedure – It is the third procedure that is often done between 2 and 4 years of age. During this treatment, surgeons will connect the inferior vena cava to the pulmonary artery.
Recovery
Commonly, after surgery, the babies should stay in a hospital for a few weeks. Most of the time, they will stay in the intensive care unit (ICU). Some of them may also need a breathing machine and a heart monitor. Doctors may also get some intravenous medicines to relieve pain and reduce the strain on the heart muscle. It is not uncommon for infants to have feeding problems. That’s why doctors often recommend a nasogastric tube or high-calorie formula instead of or along with the regular formula of your milk.
Frequently Asked Questions
When should I see my healthcare provider?
Unfortunately, once your child is diagnosed with pulmonary atresia, you will have regular follow-up appointments with the cardiologist. Usually, appointments are at least every 6 months. In general, it is very important to monitor for complications after surgery. Sometimes, children develop symptoms of heart failure, liver dysfunction, or arrhythmia after a Fontan procedure. In more severe cases, the only way to treat this condition is a heart transplant.
How long can a baby live with pulmonary atresia?
About 50% of babies with pulmonary atresia and VSD reach the age of 1, and very few of them reach 10 years of age. However, if you get treatment, people can live until their 30s.
What is the difference between pulmonary atresia and ToF?
While both are congenital heart defects, there are some differences between them. In people with pulmonary atresia, the pulmonary valve does not develop properly, but tetralogy of Fallot (ToF) is characterized by a narrowed pulmonary valve. In general, both disorders reduce blood flow to the lungs. If you have additional questions, ask your healthcare provider.