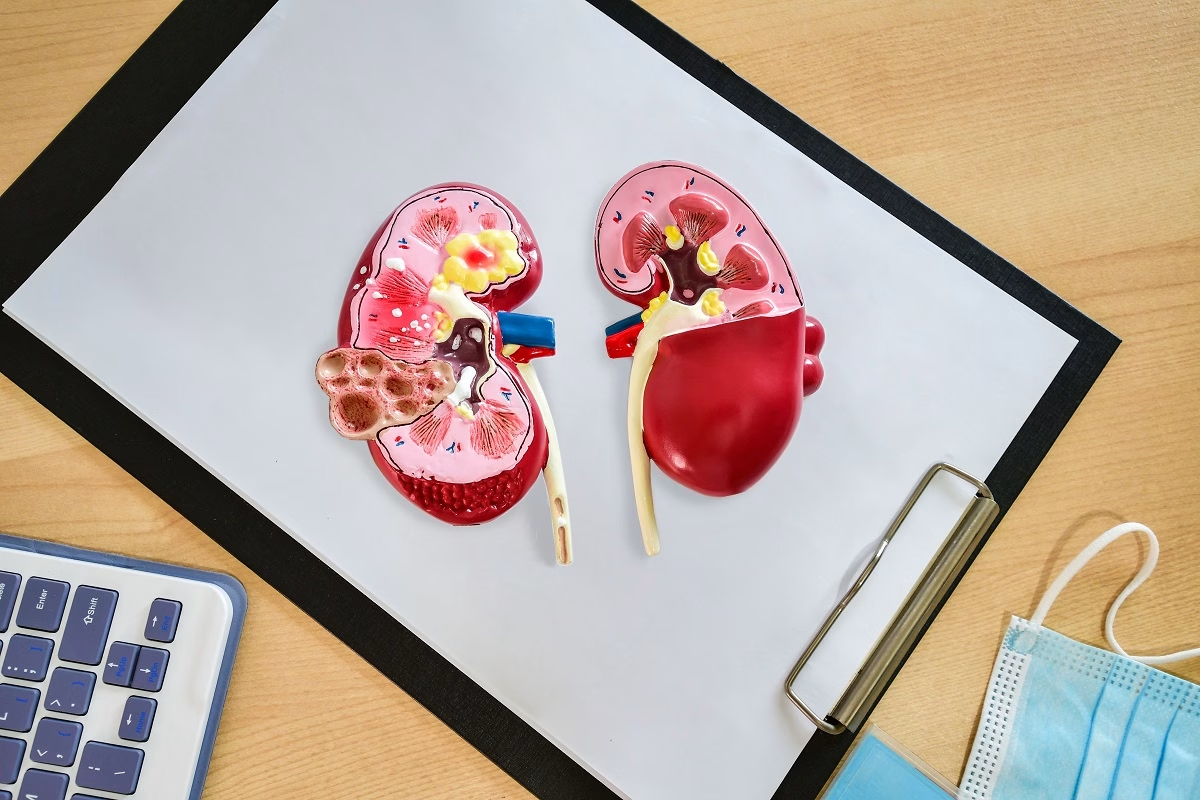
A group of health conditions that occur due to a buildup of faulty antibodies (also called M proteins) in the kidneys is called monoclonal gammopathy of renal significance (MGRS). Without treatment, the buildup of this protein can cause severe kidney damage. Usually, people who develop MGRS experience frothy or pink-tinged urine and swelling in the legs, ankles, or feet. The treatment goal is to relieve the symptoms and prevent further damage to the kidneys.
In other words, MGRS is a group of disorders that cause kidney damage due to the buildup of certain plasma cells or B cells (a type of white blood cell). Thus, plasma cells produce faulty antibodies (M proteins) that may build up in the organs and cause damage. Moreover, MGRS is not a type of cancer, but some people with this disorder may develop multiple myeloma as well as other types of cancer.
Generally, this condition occurs very rarely, and it affects less than 1% of the population. Commonly, it affects older adults (over 60 years old), but younger people may also develop it.
Types of MGRS
There are dozens of disorders that are considered types of MGRS. However, doctors have divided them into several categories based on which part of the kidney is affected by the M proteins. For example, glomerular diseases, tubulointerstitial diseases, and intrarenal vascular lesions.
Glomerular Diseases
This is one of the most common types of MGRS, and they cause damage to the small blood vessels in the kidneys. Check some examples below:
- Renal amyloidosis – It includes AL amyloidosis, AH amyloidosis, and AHL amyloidosis.
- Cryoglobulinemic glomerulonephritis (CG)
- Fibrillary glomerulopathy (FGN)
- Immunotactoid glomerulopathy (ITG)
- Glomerular diseases associated with monoclonal protein – It includes light and heavy chains deposition diseases.
Tubulointerstitial Diseases
In such cases, the following disorders negatively affect the tubes that bring filtered nutrients and fluids back to the blood (also known as tubules) and tissues around them. These include:
- Crystal-storing histiocytosis
- Light chain proximal tubulopathy (LCPT) without crystals
- Light chain Fanconi syndrome (LCFS)
Intrarenal Vascular Lesions
This type of MGRS often impacts the blood vessels of the kidneys. For instance, atypical hemolytic uremic syndrome (aHUS) is a type of MGRS in which a blood clot blocks the smallest blood vessels in the kidneys.
Symptoms
The symptoms often appear differently among people who suffer from MGRS because they depend on several factors. For example, the type and severity of the condition, age, gender, and overall health. Check below some symptoms that people who develop MGRS often experience:
- Fatigue (extreme tiredness)
- Nephrotic syndrome
- Swelling in the legs, ankles, and feet (sometimes, swelling negatively affects the abdomen, arms, or face)
- Foamy urine (this symptom can also be a symptom of proteinuria)
- Frequent urination
- Nausea
- Vomiting
- POEMS syndrome
- Hematuria (bloody urine)
- Signs of neuropathy (including numbness, tingling, or weakness)
- Discolored patches of skin
- Dyspnea (shortness of breath)
If any of the previous symptoms occur, immediately contact your physician. Otherwise, it may lead to serious complications, such as permanent damage to the kidneys.
Causes
This group of disorders causes damage to the kidneys due to a buildup of M proteins. In normal circumstances, these proteins help the body fight infections, but in people with MGRS, they do not work properly. M proteins are made up of damaged copies or clones, and certain white blood cells (including plasma cells or B cells). In some cases, people have plasma cell clones that produce M proteins without causing organ damage (monoclonal gammopathy of undetermined significance or MGUS).
Nowadays, experts do not fully understand what exactly causes these disorders. However, they think autoimmune disorders, genetic mutations (changes), infections, and certain environmental factors could play a role.
What Are The Potential Complications of MGRS?
People who develop MGRS may also experience some complications, especially if they leave it untreated. Check some of them below:
- Chronic kidney disease (CKD)
- End-stage renal (kidney) disease
- Kidney failure
- Progression to other health conditions – In some cases, people who have plasma cell clones may develop multiple myeloma. This is a type of cancer of the white blood cells. Furthermore, MGRS may also cause other types of cancer, including Waldenstrom macroglobulinemia, chronic lymphocytic leukemia (CLL), or B-cell lymphoma.
- Proteinuria
- Renal thrombotic microangiopathy (TMA) – This is a rare but serious condition that causes small vessel clotting within the kidney.
- An increased risk of recurrent MGRS
- Edema
The only sure way to prevent the previous complications is early detection and proper treatment. In any case, you can consult with your doctor about other measures to prevent them. Unfortunately, there is no way to prevent MGRS because doctors do not fully understand why it occurs.
Diagnosis
In most cases, doctors start the diagnosis of MGRS with a physical examination and questions about your symptoms and medical history to get more information about your disease. However, to confirm or exclude MGRS, doctors often perform the following tests. Examples include:
- Blood tests to check for the abnormal M protein
- Urine tests (urinalysis)
- Biopsy – During this procedure, doctors will take a sample of the affected kidney for testing. In some cases, they may also take a sample of your bone marrow for testing.
Treatment
In most cases, MGRS is treated with options similar to cancer chemotherapy. They help destroy problematic cells or stop them from producing more copies of themselves. However, physicians may also prescribe other medicines to reduce inflammation and prevent further damage to the kidneys. Check below some medicines and procedures usually used to treat people with MGRS:
- Monoclonal antibodies (such as Rituximab, Daratumumab, and others)
- Proteasome inhibitors (for example, Bortezomib, Carfilzomib, and Ixazomib)
- Immunomodulatory drugs (including Thalidomide, Lenalidomide, and Pomalidomide)
- Alkylating agents (such as Cyclophosphamide, Bendamustine, and Melphalan)
- Corticosteroids (including Prednisone and Dexamethasone)
- Autologous stem cell transplant – During this procedure, doctors will replace damaged cells with healthy ones.
- Kidney transplant – This option can be recommended by doctors in severe cases and when other options do not work.
In addition, the previous medicines and procedures may give you some adverse reactions. These include appetite changes, constipation, diarrhea, bleeding, anemia (low red blood cell count), increased risk of bacterial, viral, or fungal infections, and others.
Frequently Asked Questions
How long can you live with monoclonal gammopathy of renal significance?
Life expectancy depends on several factors. For example, the severity and type of MGRS, age, gender, existing health problems, and your response to treatment. Some studies have shown that people with amyloidosis related to MGRS live an average of 10 years after diagnosis. However, people who have had MGRS without amyloidosis lived longer.
When should I see my healthcare provider?
It is recommended to see a doctor if you have symptoms that resemble kidney problems. For example, swelling, foamy urine, frequent urination, and others.
What can I expect if I have MGRS?
While this condition is treatable, it is considered a chronic (long-lasting) condition that may return even after successful treatment. In more severe cases, when people experience permanent kidney damage, a kidney transplant is required. Furthermore, about 18% of people with MGRS also develop a type of cancer called multiple myeloma. In this case, doctors may recommend additional treatments (including radiation therapy, chemotherapy, and surgery). That’s why regular monitoring is required if you have MGRS. If you have any other questions, ask your healthcare provider.