This is a health condition that negatively affects blood flow and happens when the right iliac artery, which sends blood to the right leg, puts pressure on the iliac vein. The iliac vein carries blood from the left leg back to the heart muscle. It is called May-Thurner syndrome (MTS), and people with this condition often do not have any symptoms. Sometimes, people with MTS may develop deep vein thrombosis (DVT).
In other words, MTS interrupts normal blood flow through the legs. In some cases, this syndrome is called Cockett syndrome or iliac vein compression syndrome. Generally, this is a common condition that affects about 1 in 5 people. Moreover, a lot of people with iliac vein compression do not have a formal diagnosis of MTS because they do not experience symptoms unless DVT occurs.
How Does May-Thurner Syndrome Affect My Body?
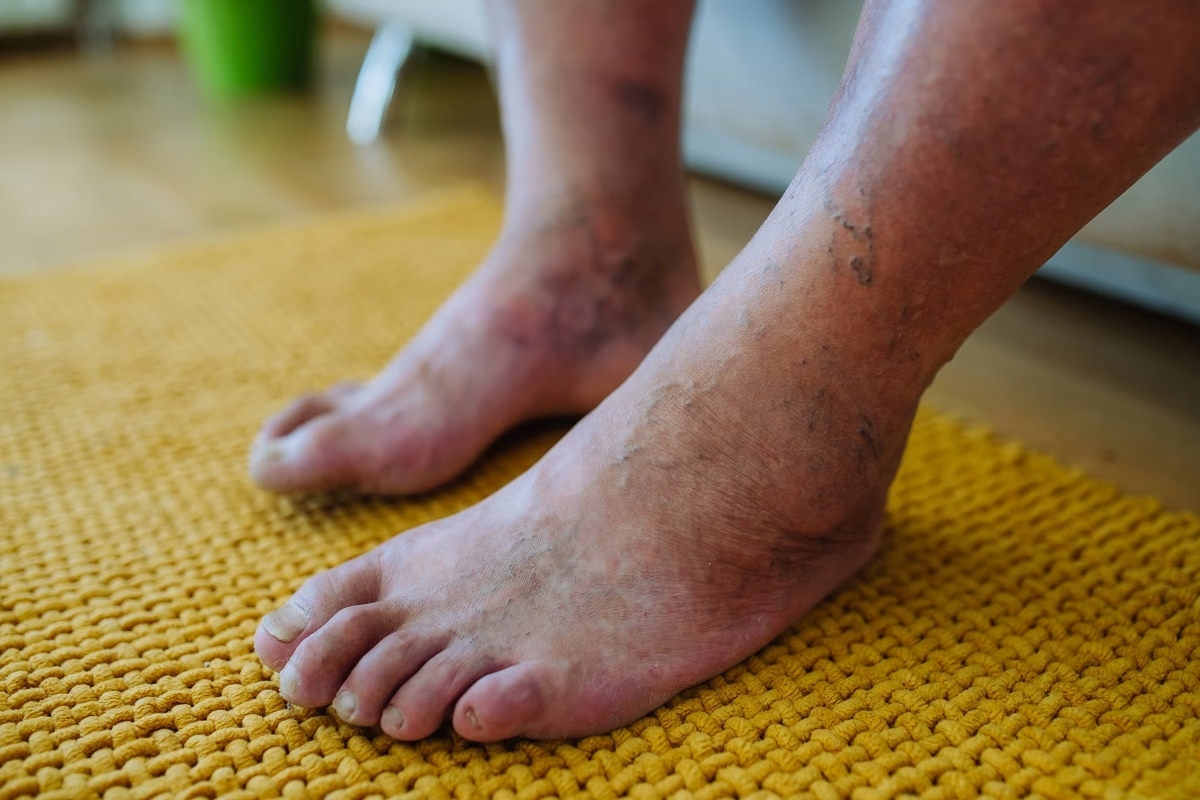
This syndrome affects the way blood flows back to the heart muscle. Instead, it may pool in the legs, which increases the risk of deep vein thrombosis (DVT). DVT happens when a blood clot forms deep in the leg veins. People with this condition often experience the following symptoms. Examples include:
- Tenderness or pain in the leg
- Enlarged and swollen leg veins
- Discolored skin on the affected leg
- Swelling in the leg
In rare cases, women with MTS may also develop pelvic congestion syndrome. According to some healthcare providers, pelvic congestion syndrome happens due to problems with the veins in the pelvic area.
Symptoms
Most people with MTS do not experience any symptoms (especially if they do not have DVT). Usually, the symptoms of MTS occur in one leg only. Check some examples below:
- Ulcers (open sores)
- Feelings of heaviness
- Pain
- Discolored skin in the affected leg
- Swelling
- Varicose veins
Do not hesitate to visit a healthcare professional if any of the previous symptoms occur.
Causes and Risk Factors
This syndrome often affects people when the iliac artery puts pressure on the left iliac vein. Nowadays, experts do not fully understand why this compression happens. However, healthcare professionals have identified some factors that may increase your risk of developing MTS. Check some of them below:
- Sex – Women between the ages of 20 and 50 are more prone to MTS.
- Anatomical factors – For example, people with scoliosis are at increased risk of developing MTS because this condition can increase pressure on the veins.
- Pregnancy – In such cases, the uterus may put extra pressure on the iliac veins (particularly during or after pregnancy). Having multiple children also increases the risk.
- Dehydration
- Lack of physical activity
- Obesity (excessive body weight)
- Hormonal imbalances – Oral contraceptives or hormone replacement therapy may also increase the risk of MTS.
- Previous pelvic or spinal surgery
- Family history – If you have a parent or sibling with deep vein thrombosis, the risk of developing MTS and DVT significantly increases.
- Blood clotting disorders (such as Factor V Leiden)
- Structural narrowing of the veins that also increases the risk of vein scarring, chronic (long-term) compression, and DVT
Complications
While the primary complication of MTS is DVT, this syndrome may also cause other complications, especially if an affected person ignores the symptoms or does not get treatment. Check for some additional complications below:
- Coughing up mucus and blood
- Heart palpitations
- Dyspnea (shortness of breath)
- Sudden chest pain that may worsen when you inhale
- Edema (swelling in the affected leg)
- Chronic leg pain
- Skin changes
- Venous ulcers
- Pelvic pain
- Pulmonary embolism – This is a serious complication that occurs when a blood clot travels to the lungs
The previous list does not contain a complete list of MTS complications. In any case, you can consult with your physician about measures to reduce the risk or even prevent the previous complications.
How to Prevent May-Thurner Syndrome?
There is no sure way to prevent this condition because physicians do not fully understand what exactly causes it. However, doctors may recommend some tips to improve blood flow and reduce the risk of blood clots. Examples include:
- Avoid prolonged periods of sitting
- Drink plenty of fluids to prevent dehydration
- Regularly perform physical exercise – You should aim for 30 minutes of physical exercise per day, at least 5 days a week. You can also perform aerobic exercise for cardiovascular health.
- Manage health conditions – These include diabetes, hypertension (high blood pressure), high cholesterol, peripheral artery disease (PAD), and others
- Stop smoking – If you have problems with smoking cessation, discuss it with your healthcare professional.
- Wear compression stockings or socks – In such cases, you should consult with your doctor whether you need them or not.
Diagnosis
In most cases, the diagnosis of MTS begins with an evaluation of your medical history and symptoms and a physical examination. However, to confirm or rule out this condition, doctors often perform the following tests and procedures. These include:
- CT (computerized tomography) scans – This is an imaging test used to make images of your blood vessels.
- MRI (magnetic resonance imaging) scans – This is another imaging test that uses a powerful magnet and radio waves to produce detailed images of different structures and organs in the body.
- Ultrasounds – These tests use sound waves to view inside the body.
- Venograms – During this test, doctors will inject a contrast dye into the veins and then use X-rays to see how the blood flows through them.
- Catheter-based venograms – During this procedure, doctors will insert a small, hollow tube (catheter) into a vein to inject the contrast dye.
- Intravascular ultrasounds – They involve inserting a catheter into blood vessels and then threading an ultrasound probe through this catheter to get detailed images of the blood vessels.
Treatment
In general, the treatment goal is to improve blood flow and reduce the risk of developing blood clots and DVT. Usually, doctors recommend the following treatment options. For example:
- Angioplasty and stenting – This treatment involves a catheter that is inserted with a balloon at the end of the iliac vein to correct its position. Therefore, doctors will inflate the balloon to open the vein. They may also insert a small mesh tube (stent) to keep the iliac vein open and remove the balloon.
- Bypass surgery – During this procedure, surgeons will take a small piece of tissue from a donor or other parts of your body to build a new route around the compressed part of the iliac vein. In most cases, it helps restore blood flow to the heart muscle.
- Surgery to move the right iliac artery – Sometimes, doctors may recommend surgery to move the right iliac artery that puts pressure on the left iliac vein. Surgeons usually place a small piece of tissue between the vein and artery to reduce pressure.
In addition, your doctor may recommend additional treatments if you develop deep vein thrombosis. Check some of them below:
- Anticoagulants (also known as blood-thinners) – This group of medicines is often recommended by doctors to prevent or dissolve blood clots.
- Clot-busting medicines – These are intravenous (IV) medicines delivered through a catheter to actively dissolve clots.
- Vena cava filter – This treatment involves a specific device that is placed in the inferior vena cava (large vein that sends blood to the heart) that traps blood clots. It helps prevent blood clots from traveling to the lungs.
Frequently Asked Questions
Is May-Thurner syndrome life-threatening?
In more severe cases, MTS can cause pulmonary embolism, which is a life-threatening complication. Immediately call 911 or go to the nearest emergency room (ER) if you have pulmonary embolism symptoms.
How do you tell if you have May-Thurner syndrome?
Usually, people are not able to tell they have MTS until DVT occurs. The only way to diagnose this condition before DVT is imaging tests that can show a compressed iliac vein.
What can I expect if I have May-Thurner syndrome?
Most people with MTS live long and healthy lives. Sometimes, they may not even know they have this syndrome because it does not cause any symptoms. However, the symptoms may begin to appear when a person develops DVT. Generally, there are a lot of people who successfully treat DVT with medicines (such as anticoagulants). Ask your healthcare provider if you have any other questions.